The importance of posture
This article explains why good posture is essential, especially for people with cystic fibrosis, and offers concrete strategies to prevent pain, musculoskeletal complications, and maintain respiratory function.
The term posture describes the position of the body and the relationship that exists between each of its components. Every day, every minute, the body adopts different postures, which can be static — such as when resting or sleeping — or dynamic — such as when walking or doing sport1. Any posture involves the muscles, joints, nerves, and connective tissues of the body. A posture can become painful because of the pressure it exerts on some or all of these components. It is influenced by multiple factors, including mood (have you ever noticed that your shoulders sag when depressed?) , environment, gender, general health and personal habits.
What is the ideal posture?
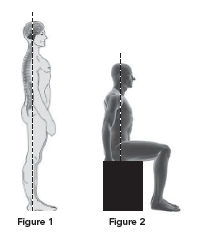
An ideal posture allows the body to maintain a position without putting undue pressure on any part of the bone or any muscle. For example, when standing, the head should be in a neutral position and the shoulder blades should lie flat against the back, the spine should follow its natural curves, and the knees should not be locked in hyperextension (see Figure 1). A simple way to check if you have a good standing or sitting posture is to imagine that a plumb line runs through your entire body, as shown in figures 1 and 2.
Why is it important to think about your posture?
Good posture is in everyone's best interest because it can prevent injuries and pains in daily life. Having a good sitting posture during periods of study or work helps to prevent back and nuchal muscle tensions that can cause pain. Since you spend a lot of time lying down, it is essential to ensure that your mattress and pillow offer optimal support and comfort.
Link to cystic fibrosis (CF)
Research has shown that people with CF are at high risk of poor posture and pain, and are more likely to develop osteoporosis or osteopenia (reduced bone mineral density), which can cause pain and require postural corrections. Risk factors for the development of muscular and bone complications leading to poor posture include reduced FEV1, low lean body mass, diabetes associated with FK6, corticosteroid treatment, pancreatic insufficiency, physical inactivity, physical inactivity, physical inactivity, vitamin D deficiency, vitamin D deficiency, chronic lung infection, late puberty, and the presence of the ΔF50814 genotype. Research is ongoing to determine whether the defect in the CFTR protein that causes CF (and which has been identified in bone cells) is the main cause of bone complications, especially the loss of bone mineral density, or if postural problems are a secondary complication of the disease. In addition, it has been observed that the muscular strength of CF patients is often lower than that of the general population; scientists are trying to find out whether this situation is specific to the defect in the protein responsible for CF or whether it stems from the lack of activity and muscle training, which is a consequence of the complications of the disease. It has been suggested that the weakening of expectoration and breathing functions, the inflammatory reactions, and the decrease in the frequency of physical activity that accompany lung infections are the main culprits of postural complications. Repeated lung infections can alter lung function and worsen breathing difficulties. The core muscles work to facilitate breathing while helping to maintain posture; therefore, the more they are called upon for respiratory function, the less they can support posture. This situation subjects the bone to postural complications or even deformities due to excessive forces exerted, for example when the person coughs or is in a stooped position for an extended period of time. Prolonged infections or periods of inactivity can cause soft tissue such as muscles to adapt to non-ideal resting postures. For example, if the muscles in the rib cage are shortened as a result of a sitting posture where the back is arched and the shoulders are rounded, it is difficult to straighten the spine and sit up straight. In this case, it can be painstaking to get your shoulders to play freely and breathe deeply. Long-term consequences of this posture include a poorer ability to perform bronchial cleaning and spirometric tests, as well as a decrease in the ability to exercise, which can create a vicious cycle that puts the person at greater risk of contracting respiratory infections and making their health even worse.
What do we mean by postural complications?
Postural complications often result from soft tissue changes, such as changes in muscle length due to adaptation to a non-ideal posture, which can reduce flexibility or range of motion. In people with cystic fibrosis, the parts of the body that are usually affected are the shoulders, rib cage, and upper back. Impaired muscle function instill a new sense of applying force or compromises the support of the bones to which the muscles are connected, pulling them in non-ideal directions, which can lead to bone deformities such as increased lordosis (called round back or dorsal kyphosis), which places the spine at risk of vertebral fractures.16 Pain can occur at any stage of these changes as the body adapts to these changed positions and as the range of motion decreases. Sources of discomfort include pain points in shortened muscles, pressure on weak points in the skeleton, and hyperextension of body parts in non-ideal positions.
People at risk
Postural abnormalities are more common in aging cystic fibrosis people whose disease is progressing, especially those who are more prone to respiratory infections and coughing attacks. To date, there are no studies that reveal the presence of postural abnormalities in children under the age of six. On the other hand, numerous studies have reported the emergence of musculoskeletal abnormalities in prepubertal children, and these were mainly related to the loss of bone mineral density. As for the adult population, pain caused by postural adaptation is increasingly observed, more precisely lower back pain; some studies even go so far as to put this frequency at 94% in this group of patients.
In the adult non-cystic population, the prevalence of low back pain over the lifespan would be 50 to 80%, which suggests that CF patients are more likely to experience low back pain. With the encouraging prospect of longer lives for people with CF, it is likely that we will see more postural complications due to CF related bone diseases that accompany the wear and tear caused by aging and living a more active lifestyle. It is therefore important for anyone with CF to be aware of the likelihood of developing postural complications and to know what to do about them.
What to do?
The loss of bone mineral density is linked to postural complications, which is why it is crucial to strictly adhere to vitamin D and calcium intake, since these supplements contribute to the construction and maintenance of strong bones. Approximately 90% of adult bone mineral density is acquired during adolescence; as bone mass peaks between the ages of 20 and 30, it is at this age that it is important to strengthen bone mass. The prevention of bone diseases and postural complications therefore involves consulting your CF clinic dietitian, who will optimize the dose of vitamin and mineral supplements, and maintaining a healthy weight.
In the population without CF, weight-bearing exercises (e.g., jumping) have been shown to promote optimal bone mass, strength, and size while limiting bone loss. Research has proven the beneficial effects of weight-bearing exercise on the bones of young adults, effects that can last into adult life. A group of specialists in bone diseases related to cystic fibrosis has written a consensus document that recommends that patients with cystic fibrosis practice weight-bearing exercises in order to mitigate the effects of bone diseases.
The best way to combat postural complications is to prevent them from happening, to always be aware of your posture and to stretch after being in a non-ideal posture; these are simple tips that will allow you to adopt a good posture on a daily basis. It can also be very useful to ask your physiotherapist for advice, as he can suggest positions to optimize your posture that can be combined with nebulizer therapies or bronchial toilet techniques. Remember to have your posture checked during the annual exam with the CF team. It can draw attention to neuralgic regions or suggest exercises to correct a non-ideal posture or stretching for tense muscle groups. Often, it is possible to correct your posture yourself in everyday life without increasing the treatment burden. If the problems get worse, for example if you experience low back pain due to reduced spinal mobility, manipulative treatment may be effective in relieving the discomfort. Your physiotherapist will assess the need for these types of interventions.
Action plan to adopt an optimal posture
1. Evaluate your posture
You can self-assess your posture by sitting or standing in front of a mirror. Next, imagine a plumb line running through your body from head to toe (figures 1 and 2) and try to adjust your position to match the ideal posture. Talk to your physiotherapist about your posture and ask them to check it; they can then help you develop a posture management plan, which can include a range of interventions from being aware of your posture throughout the day to engaging in targeted exercises that treat problem areas.
2. Optimize your diet
Communicating with your CF Clinic dietitian is essential to ensure that your diet is optimal for bone health. Among other things, make sure that your diet contains the appropriate doses of vitamin D and calcium or take supplements that you have been prescribed, as well as maintaining a healthy weight; all of these measures will help you prevent postural problems.
3. Do activities with charge
Regardless of your age, weight-bearing exercises are known to contribute to bone health, which helps prevent postural complications. Two types of exercises are particularly recommended: exercises with dynamic load such as jumping or those with irregular load such as ball games or gymnastics, which involve numerous sudden changes of direction. To use all parts of the body, you will need to vary the muscle group that carries the load: for example, to strengthen your upper muscles, support the weight of your body with your arms as during yoga or gymnastics exercises; to strengthen your lower muscles, make your lower muscles carry the weight by your legs by practicing jumps. Remember that these activities also benefit your respiratory capacity and general health, allowing you to improve several functions at the same time!
4. Maintain your flexibility
The body is able to maintain ideal postures without difficulty when its muscles can contract optimally. By improving the flexibility of your muscles, you can have a good posture in addition to preventing pain caused by unequal traction exerted on the skeleton due to tight muscles. Stretch well after exercising to prevent muscle groups from shortening. Yoga and Tai Chi are known to improve posture, strength, and flexibility while providing positive effects on mood and possible benefits for bone mineral density
5. Prevent injuries
If you suffer from a loss of bone mineral density or osteoporosis (which your medical team will have diagnosed after an examination by ADEX), it is important to continue exercising while being careful not to expose yourself to the risk of injury. Just follow these few simple principles: avoid exercises or activities that involve curving, flexing, or twisting the spine and limit high-load exercises to reduce the risk of bone fractures. It is recommended that you consult a physical activity specialist or physical therapist for advice on how to properly progress with activity, how to stretch and strengthen muscles without injury, and how to correct poor postural habits.
Gemma Morgan, physiotherapist specializing in adult cystic fibrosis
NHS Foundation Trust, Royal Brompton & Harefield Hospital, London (UK)
Health
Thanks to Our Partners























