Understanding Cystic Fibrosis
Cystic fibrosis is a genetic disease that makes mucus thick and sticky, mainly affecting the lungs and digestion, but modern treatments now make it possible to live better with the disease.

Cystic fibrosis (CF) is an inherited condition that causes functional disorders in a group of glands called exocrine glands. Exocrine glands normally produce clear, fluid secretions. In people with CF, these secretions are thick and viscous. The disorders caused by CF are mainly related to the respiratory and digestive systems, in addition to affecting other systems.
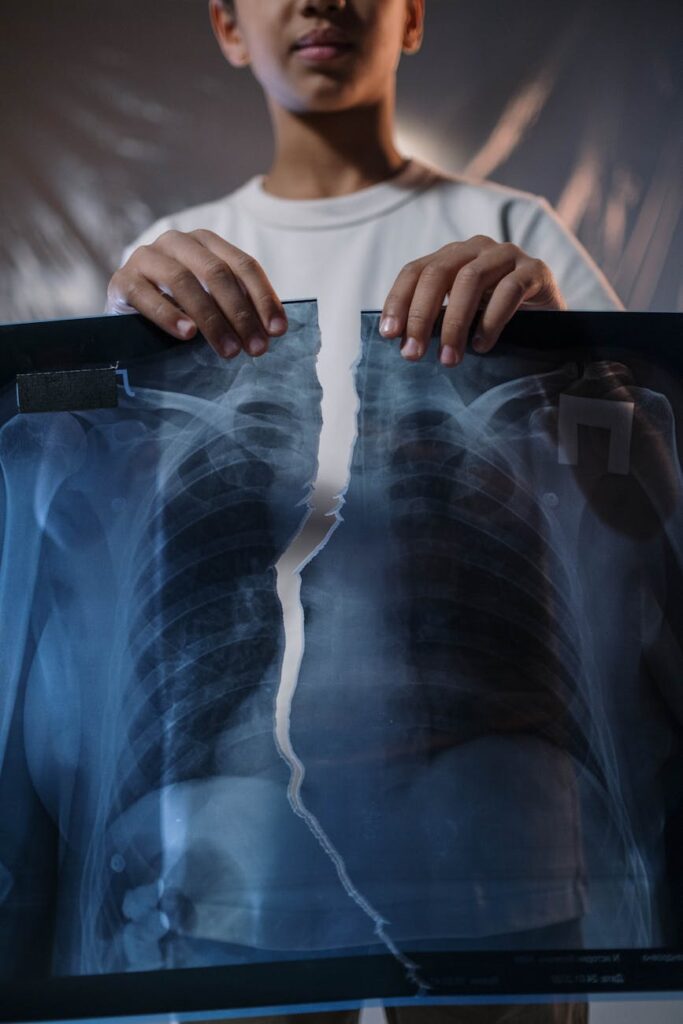
In people who don't have CF, the glands in the walls of the lung's airways produce clear, fluid mucus for a specific purpose: to help trap the dust and bacteria we inhale every day. Clear mucus is carried upward by vibratory hairs (called cilia) to the trachea, where it can be expectorated or swallowed. In lungs affected by CF, the mucus is thick and viscous, and it is more difficult for the cilia to carry it out of the lungs. Thick mucus builds up in the airways and obstructs them. This can lead to air retention, airway obstruction, and infections.
Thick mucus can also block the ducts of the pancreas. The pancreas is a gland located under and behind the stomach. It is one of the essential organs of the digestive tract. It provides the enzymes that are essential for digesting food. If the holes in the pancreas are obstructed, the enzymes cannot reach the small intestine. As a result, foods are only partially digested and their nutritional value is reduced. In fact, 85% of people with CF don't secrete enough enzymes to fully digest food. This leads to weight loss and growth problems.
Symptoms
Because CF affects more than one system in the body, a person with CF may experience a variety of symptoms. Here is a list of the most common symptoms:
- Persistent cough that produces thick mucus
- Weight loss or inability to gain weight
- Salty-flavored skin
- Stools that are generally excessive, bulky, and foul-smelling
- Frequent lung infections, which may include pneumonia
- Wheezing and shortness of breath
- Digital hippocratism
- Infertility or reduced fertility
Parents usually give the doctor the first clue in diagnosing cystic fibrosis in their child. Indeed, the salty taste of a child's skin when kissed is quickly noticeable.
Other symptoms include a persistent cough similar to that of whooping cough, wheezing that can be mistaken for asthma, recurrent lung infections, such as bronchitis or pneumonia, failure to grow and gain weight despite a great appetite, and frequent, bulky, and foul-smelling stools. Coughing can become so persistent that it interferes with a child's sleep and feeding and may even cause vomiting.
Abdominal distension may be another manifestation of cystic fibrosis. However, if it is the only symptom, it is probably not necessarily a sign of the disease, because a plump tummy in small children is common. Sometimes, bulky stools in children can cause the rectum to relax (rectal prolapse). Abdominal pain, on the other hand, is occasional and results from the accumulation of gas caused by poor digestion of food.
Cystic fibrosis is not always identified in children. Indeed, sometimes the symptoms do not appear very clearly. In addition, chronic diarrhea, breathing difficulties, and other symptoms of cystic fibrosis can be attributed to other illnesses.
An easily identifiable manifestation of cystic fibrosis is meconium ileus, an intestinal occlusion that occurs when the intestines are blocked by secretions that have the consistency of a sealant. The result is abdominal bloating, vomiting, and the inability to have a bowel movement. Medical therapy is effective in many of these cases, and surgery is used for complicated cases.
Diagnosis
The symptoms of cystic fibrosis can sometimes be mistaken for other conditions. As already mentioned, coughing can be associated with whooping cough, and wheezing can be associated with asthma. When a child develops pneumonia or bronchitis, cystic fibrosis is not always recognized as the root cause of the condition. Likewise, various common digestive problems resemble the digestive symptoms of cystic fibrosis.
If there is a suspicion of cystic fibrosis, a “sweat test” is often the first test performed. This test analyzes the salt content in sweat. High salt content is an important indicator of the possible presence of CF. A person may or may not have other symptoms.
A genetic analysis based on a blood sample is also used to confirm the diagnosis of CF. There are over 1800 mutations in the gene responsible, but people are generally tested for 30 of the most common ones. Prenatal genetic tests may be done to make the diagnosis.
If the doctor suspects that the child may have cystic fibrosis, the doctor will order special tests to make sure. In this regard, a “sweat test” is often performed, which involves stimulating an area of the skin with heat or medication. If the salt content in sweat is higher than normal, the diagnosis of cystic fibrosis may be considered. A test to detect the presence of enzymes in the intestines may also be performed. Likewise, the doctor will inquire about the child's digestive problems and breathing difficulties, infections, and weight gain problems. He will often order a chest X-ray to determine changes in the condition of the lungs. Putting together thuis information, the doctor will arrive at a diagnosis.
In addition, a genetic test, undertaken on a blood sample, can confirm the diagnosis. A cure for cystic fibrosis does not yet exist, but effective treatment methods are available. Currently, more and more young people are reaching adulthood without having suffered too much lung damage. The discovery of the gene responsible for cystic fibrosis also promises even more advanced treatment methods. With the discovery of this gene, researchers can, for the first time, trace the links between the cause of this condition and all of its signs and symptoms.
Causes
The functioning of healthy lungs
- Your lungs are made up of lots of parts that work together to help you breathe.
- Each lung is divided into sections called lobes.
- When you inhale (or breathe in), air enters the trachea. It circulates through small airways (bronchi and bronchioles) to very small air bags located inside the lungs (the alveoli).
- It is in the alveoli that oxygen from the air you inhale passes into the bloodstream. At the same time, carbon dioxide leaves the bloodstream to be eliminated with the air you exhale (or breathe out).
Lungs affected by cystic fibrosis
- The airways in your lungs are covered by a layer of mucus, a protective coating that is constantly replenished by lung cells.
- Humans have a gene responsible for the production of CFTR, a protein that regulates transmembrane permeability. People with cystic fibrosis have abnormal copies of this gene. It is believed that these abnormal genes are responsible for the secretion of dehydrated mucus, which is very difficult for the lungs to clear.
- This viscous, stagnant mucus obstructs or blocks the airways (making it difficult to breathe) and provides an ideal site for infectious bacteria to multiply.
Cystic fibrosis occurs in children who inherit two copies of the defective gene, one from each parent. A parent whose cells have only one copy of the gene cannot have cystic fibrosis. But when two people who each have this gene have children, one or more of their children can inherit both genes and be born with cystic fibrosis.
In this case, for each birth, there is a 25% chance that the child will have cystic fibrosis, a 50% chance that the child will be a carrier, and a 25% chance that the child is neither affected nor a carrier. In Canada, in 2008, cystic fibrosis affected one in 3,600 newborns. Geneticists estimate that one in 25 Canadians carry the gene responsible for cystic fibrosis.
In Quebec, this proportion is 1 in 20 people. Generally, the parents of a child with cystic fibrosis do not have the disease. They often don't know that they carry the gene, and don't understand how they were able to pass it on to their baby. In August 1989, Canadian researchers discovered the normal gene that, when mutated, causes cystic fibrosis. If a child inherits one copy of this defective gene from each parent, some cells in their body will produce a protein that will not function normally.
Cystic fibrosis is not contagious and is therefore not transmitted from one child to another.
Researchers are currently working to define the exact role of this protein. What is certain so far is that it impedes the movement of salts and fluids across the membranes of affected cells. This action produces the characteristic symptoms of cystic fibrosis, namely the accumulation of thick, dry mucus in the lungs and the obstruction of the pancreatic ducts. Cystic fibrosis is a hereditary disease and does not depend on the surrounding environment.
The birth order of the child, the age of the parents, or the mother's diet during pregnancy do not determine whether or not the newborn will have cystic fibrosis. Cystic fibrosis is not contagious and is therefore not transmitted from one child to another.
Treatments
Lung treatments
The treatment of cystic fibrosis focuses primarily on lung problems, as the disease itself and associated mortality are mainly attributed to infection and poor lung function. The aim of lung treatments is to loosen and remove mucus that obstructs the airways in order to achieve good lung function. A number of methods are used. Taking antibiotics frequently helps fight and prevent lung infections. Special aerosol solutions are used to loosen mucus in the lungs and make it more fluid. In addition, postural drainage with “clapping”, a form of physiotherapy where the individual is placed in different positions chosen according to the area to be drained to apply pressure to the lobes of the lungs, helps to unblock the airways. This method often allows a large quantity of mucus to be evacuated. Other drainage techniques, which do not require the assistance of a third party, ensure greater autonomy for the patient. Among other things, these include “huffing” and autogenous drainage. In very severe cases, the lungs become so damaged as a result of repeated infections that the only solution is a transplant.
Gastrointestinal treatments
The gastrointestinal disorders of cystic fibrosis appear in around 85% of those affected in the form of poor digestion and malabsorption of fats, proteins and carbohydrates. Before treatment, an affected person may consume twice the amount of food consumed by a normal person. People with cystic fibrosis generally need to take special pancreatic enzyme supplements to aid digestion, follow a special diet high in calories and protein, and supplement their diet with vitamin supplements containing vitamins E and sometimes vitamin K. Pancreatic enzymes taken orally make up for most of the deficits caused by the disease. They help the body absorb nutrients and reduce the amount and volume of stools, the amount of gas that builds up, abdominal pain, and distension. In addition, people with cystic fibrosis are forced to add salt to their diet in order to replace the large amount lost in their sweat.
Contamination
We have an infection prevention policy: this is the Hygiene, Cross-Contamination and Infection Prevention Policy. We invite all our members — as well as those who are called upon to come into contact with people living with cystic fibrosis — to read it without delay and to implement the basic instructions it contains. To ensure compliance with these hygiene rules during meetings and events organized by Living with Cystic Fibrosis, we invite participants to sign a personal commitment form in favor of infection prevention.
Hygiene, Cross-Contamination, and Infection Prevention Policy
External resources
Health Info: 811
Free and confidential telephone consultation service with nurses, available 24/7 for non-urgent health problems. Provides advice and referrals to appropriate resources.
Thanks to Our Partners























.jpg)